How to Test My Testosterone Levels & Understand Results
This article shows you how to test your testosterone levels. Learn the difference between at-home kits and lab tests, what they cost, and what your results mean.

This content is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider for any health concerns or before making any decisions related to your health or treatment.
Feeling off? Maybe you’re dealing with constant fatigue, a lagging libido, or trouble building muscle no matter how hard you work in the gym. These can be signs of low testosterone. The first step toward getting answers is understanding exactly how to test my testosterone levels the right way. An incorrect test can give you a false sense of security or lead you down a path of unnecessary treatment.
This guide will walk you through the entire process, step by step. We'll cover what you need to know before you start, how to prepare, what tests to ask for, and how to make sense of the results you get back. Getting this right from the beginning is the key to an accurate diagnosis and effective planning with your doctor.
What You'll Need
Before you can get your testosterone levels checked, you'll need a few things in place. Think of this as your pre-test checklist.
First, you need a way to order the test. This can happen in three main ways:
- Through your doctor: A primary care physician or an endocrinologist can order lab work for you.
- Direct-to-consumer (DTC) labs: Companies allow you to buy a lab test online, go to a local draw center (like Quest or Labcorp), and get your results directly.
- At-home test kits: These kits are mailed to you, and you collect a sample (usually blood via a finger prick or saliva) and mail it back to a lab.
Second, you'll need to budget for the test. Costs can vary significantly. A simple Total Testosterone test might cost between $69 and $130, while a more complete panel can range from $159 to $220 if you pay out of pocket (BetterCare, 2026). Insurance coverage depends on your plan and whether the test is deemed medically necessary by your doctor.
Finally, you need a clear understanding of what a good test involves. This includes the right timing, proper preparation, and the specific markers that give you a full picture of your hormonal health.
Before You Start
Knowing how to test your testosterone levels properly is more than just getting your blood drawn. Several factors can dramatically affect your results, and getting them wrong can lead to a misdiagnosis.
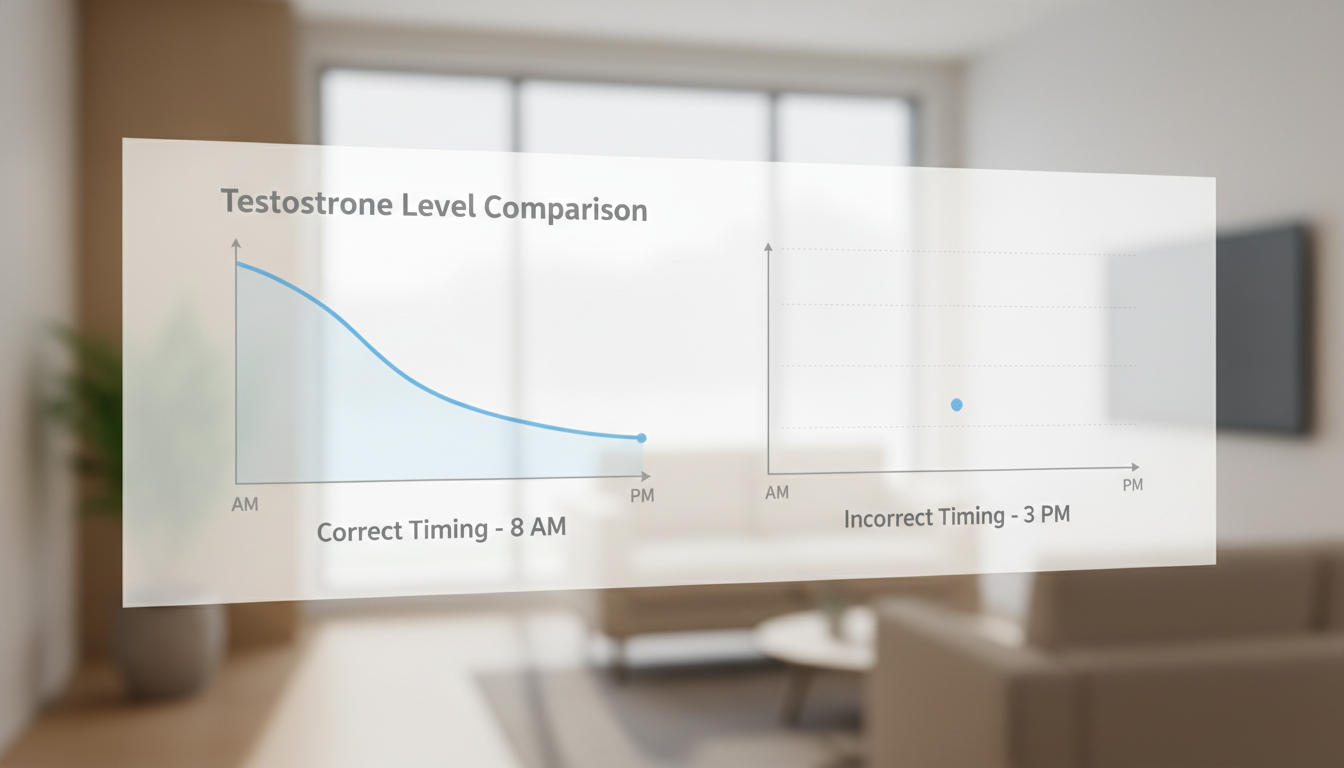
The single most important factor is timing. Your testosterone levels follow a natural daily rhythm, peaking in the morning and declining throughout the day. For this reason, all official guidelines recommend scheduling your blood draw for the early morning, ideally between 7 AM and 11 AM (The TRT Catalog, 2026). A test taken in the afternoon could show a falsely normal or low level, making it useless for diagnosis. The Well by Northwell Health notes that a single, ill-timed test is a common cause of misdiagnosis.
Next is preparation. To ensure your test reflects your true baseline, you need to prepare for 24 to 48 hours beforehand. This includes:
- Fasting: You should fast for 8-12 hours before your blood draw. This means nothing to eat or drink except water.
- Avoiding intense exercise: Strenuous workouts can temporarily alter your hormone levels. Avoid them for at least 24 hours before your test.
- Skipping alcohol: Alcohol can also impact your hormone production, so it's best to avoid it for a day or two prior.
- Getting good sleep: Poor sleep or sleep deprivation can lower your testosterone levels, so aim for a full night's rest before your test (The TRT Catalog, 2026).
Finally, you need to know that a single test is not enough for an official diagnosis. Both the American Urological Association (AUA) and the Endocrine Society state that a diagnosis of Testosterone Deficiency requires two separate morning blood tests confirming low levels, along with corresponding symptoms (AUA Guideline; Highland Longevity, 2026).
Feeling overwhelmed by the options and preparation? It can be a lot to manage on your own. If you want guidance on finding a provider who can handle the testing process for you, our free quiz can help.
Take our free 3-minute quiz to get matched with a provider who can manage your testosterone testing.
Step-by-Step Guide: How to Test My Testosterone Levels Accurately
Follow these steps to ensure you get a clear and accurate reading of your hormone levels.
Step 1: Recognize the Symptoms of Low Testosterone
Before you even order a test, it’s helpful to understand if your symptoms align with low testosterone (also known as hypogonadism). Hormones affect nearly every system in your body, so the signs can be widespread. Common symptoms include:
- Low sex drive (libido)
- Erectile dysfunction (ED)
- Persistent fatigue and low energy
- Loss of muscle mass and strength
- Increased body fat, especially around the waist
- Depressed mood or irritability
- Difficulty concentrating or "brain fog"
- Loss of body or facial hair
Having one of these doesn't automatically mean your testosterone is low. However, if you're experiencing a combination of these issues consistently, it's a strong signal that testing is a logical next step. Documenting your symptoms will also be extremely helpful when you discuss your results with a healthcare provider. They will need to see both low lab numbers and consistent symptoms to make a proper diagnosis, as recommended by the AUA. The real goal is to improve how you feel, and the blood test is just one tool to figure out how.
Step 2: Choose Your Testing Method
You have three primary options for getting your blood work done, each with its own pros and cons.
-
Through a Doctor: This is the traditional route. You visit your primary care physician or a specialist like an endocrinologist, discuss your symptoms, and they order the lab work.
- Pros: Often covered by insurance (costs could be as low as $0-$50 copay). A doctor guides the process.
- Cons: Your doctor might only order a basic "Total Testosterone" test, which can be insufficient. You may also need multiple appointments, which takes time.
-
Direct-to-Consumer (DTC) Labs: Services like those offered by many telehealth platforms allow you to order comprehensive hormone panels online. You pay a flat fee, receive a lab requisition form, and visit a nearby patient service center (like Quest Diagnostics or Labcorp) for the blood draw.
- Pros: You control which tests you get. The panels are often more detailed than what a GP might order initially. It's confidential and often faster.
- Cons: Usually not covered by insurance. Costs can range from $120 to over $200 for a good panel (The TRT Catalog, 2026).
-
At-Home Test Kits: These kits are ordered online and sent to your home. You collect a sample, typically through a finger-prick blood sample or a saliva sample, and mail it to a lab.
- Pros: Maximum convenience and privacy.
- Cons: The accuracy of finger-prick and saliva tests can be less reliable than a venous blood draw done at a lab (Highland Longevity, 2026). They are useful for a general snapshot but are not typically used for a formal diagnosis.
For a definitive diagnosis, a venous blood draw handled by a professional phlebotomist is the gold standard.
Step 3: Schedule the Test and Prepare Correctly
Once you've chosen your method, scheduling and preparation are critical. As mentioned, your testosterone levels are highest in the morning.
Schedule your appointment for as early as possible, ideally between 7:00 AM and 10:00 AM. According to Veedma, this timing is crucial for an accurate reading. When you book, confirm the time. Don't let the lab schedule you for an afternoon slot.
Next, lock in your preparation plan for the 24-48 hours leading up to the test:
- Start Your Fast: Plan to stop eating and drinking anything other than water about 8-12 hours before your appointment. If your draw is at 8 AM, you should stop eating around 8 PM the night before.
- Plan Your Exercise: Make the day before your test a rest day. Avoid any strenuous exercise, including heavy weightlifting or intense cardio.
- Avoid Alcohol and Sex: For the most accurate results, avoid drinking alcohol and sexual activity for at least 24 hours, or even 2-3 days if possible (Veedma, 2026).
- Prioritize Sleep: Do your best to get a full, restful night of sleep. High stress and poor sleep can temporarily suppress your testosterone levels (The Well, Northwell).
Following these steps minimizes the external factors that could skew your results and ensures the lab report reflects your body's true hormonal state.
Step 4: Select a Comprehensive Hormone Panel
Simply asking for a "testosterone test" is not enough. You could end up with a single number for Total Testosterone, which doesn't tell the whole story. To truly understand how to test my testosterone levels, you must ask for the right panel of tests.
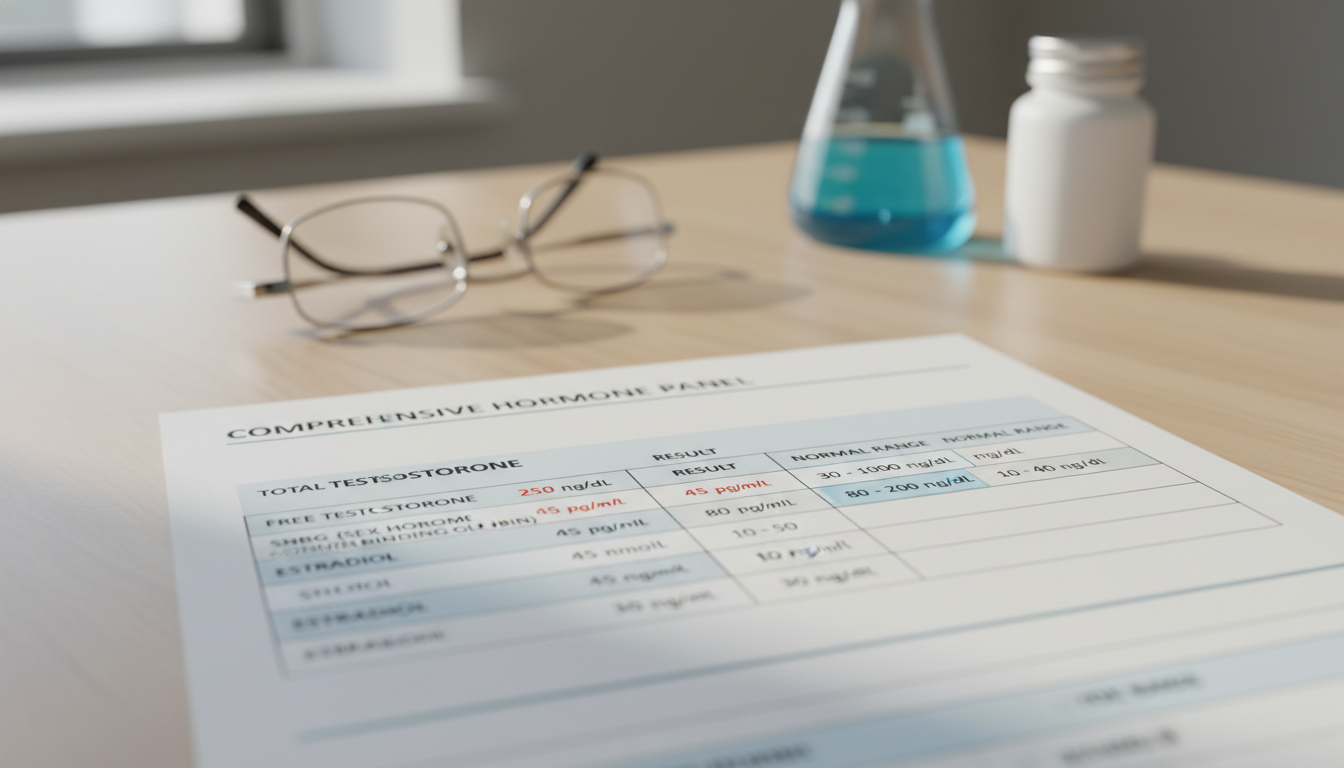
Here’s what a good baseline panel should include:
- Total Testosterone: This measures the total amount of testosterone in your blood, including testosterone bound to proteins and "free" testosterone. The AUA uses a cutoff of 300 ng/dL as a general guideline for low T.
- Free Testosterone: This measures the testosterone that is not bound to proteins and is biologically active, meaning it's available for your body to use. This is a critical marker because some men can have normal Total T but low Free T, which could still cause symptoms. Up to 30% of men with symptoms fall into this category (Compare Men's Care, 2026).
- Sex Hormone-Binding Globulin (SHBG): This is a protein that binds to testosterone, making it inactive. High SHBG can lead to low Free Testosterone even if your Total T is normal.
- Luteinizing Hormone (LH) and Follicle-Stimulating Hormone (FSH): These hormones are produced by your pituitary gland and signal your testes to produce testosterone. Measuring them helps determine the cause of low testosterone (primary vs. secondary hypogonadism).
- Estradiol (Sensitive Assay): Men also need estrogen, but in the right balance. High estradiol can cause symptoms similar to low testosterone. A "sensitive" assay is required for the low levels found in men.
A complete panel gives you and your doctor a full dashboard of your hormonal health, not just a single gauge. If you're using a DTC lab, these comprehensive panels are usually standard. If going through a doctor, you may need to specifically request these additional markers.
Step 5: Get Your Blood Drawn
This is the simplest step in the process. You’ll go to the lab or your doctor's office at your scheduled appointment time. A phlebotomist (the person trained to draw blood) will clean an area on your arm with an alcohol wipe, insert a small needle into a vein, and collect one or more vials of blood.
The process is quick, usually taking less than five minutes. It can be slightly uncomfortable, but it's generally not painful. Afterward, they'll place a bandage on the spot, and you can go about your day. Since you were fasting, it's a good idea to bring a snack and some water to have right after your draw is complete.
Results are typically available within 2-5 business days (BetterCare, 2026). If you went through a doctor, their office will call you. If you used a DTC lab or telehealth service, you'll likely receive an email to view your results in a secure online portal.
Step 6: How to Read and Understand Your Results
Receiving your lab report can feel intimidating. It will be pages of numbers, acronyms, and "reference ranges." Don't try to diagnose yourself. These results are meant to be discussed with a qualified healthcare provider. However, you can learn to understand the key numbers.
- Total Testosterone: Look for this number first. According to the AUA, a level below 300 ng/dL is a common threshold for considering a diagnosis, though some providers use different ranges.
- Free Testosterone: This is often measured in pg/mL. Levels below 100 pg/mL are often considered low, especially in men with symptoms (Veedma, 2026).
- Reference Ranges: Your report will show a "reference range" next to your result. These ranges represent the "normal" spread for a large population. However, "normal" isn't always "optimal." A level that is technically within the normal range but on the low end could still be the cause of your symptoms.
Remember, a single test is not enough. Abnormal results, whether high or low, do not automatically confirm a serious condition (Cleveland Clinic). Your doctor will need to see two separate morning tests showing consistently low levels, combined with your symptoms, to make an official diagnosis. If low T is confirmed, the next discussion is often about treatment. This is where you can learn more about the pros and cons of different approaches, from tablets to injections and the real testosterone injection benefits.
Wondering what to do with your results or how they fit into a larger treatment plan? It’s often best to work with a specialist.
Find a vetted hormone specialist near you by taking our free 3-minute quiz.

Demystifying the Process: How to Test My Testosterone Levels Without Confusion
Trying to figure out how to test my testosterone levels can feel complex, but it boils down to a few key principles. The goal is to get a reliable baseline reading that you and your doctor can trust. A hasty or poorly planned test is often worse than no test at all because it can provide misleading information.
The most important takeaway is that timing and preparation are everything. A non-fasted, afternoon blood draw is essentially useless for diagnosing low testosterone. You must commit to an early morning, fasted test to get accurate data.
Furthermore, context is key. A number on a page means very little without the full picture. That picture includes your age, your specific symptoms, your overall health, and other hormone markers like Free T, SHBG, and Estradiol. This is why a comprehensive panel is so much more valuable than a simple Total T test. If your results come back in the "low-normal" range but you feel terrible, that's a conversation worth having with a provider who specializes in hormone optimization. They can help you understand what your TRT before and after results could look like. Finding the right path starts with getting the right data.
Common Mistakes to Avoid
Many people make simple mistakes that invalidate their test results. Here are the most common ones to watch out for:
- Testing in the Afternoon: This is the number one error. Testosterone levels can be up to 30-40% lower in the afternoon. A test taken at 3 PM could make a man with genuinely low T appear normal. Always test before 11 AM.
- Only Testing Total Testosterone: As mentioned, 20-30% of men with low T symptoms have normal Total T but low Free T (Compare Men's Care, 2026). Without measuring Free T and SHBG, you miss a huge piece of the puzzle.
- Relying on a Single Test: Hormone levels can fluctuate daily due to sleep, stress, or illness. All clinical guidelines require at least two separate low readings on different days for a diagnosis.
- Not Fasting: Eating before your test can affect blood glucose and other markers that can indirectly influence hormone readings. An 8-12 hour fast is standard procedure.
- Exercising Before the Test: A heavy workout can temporarily suppress or sometimes spike hormone levels, leading to a confusing result. Take a rest day before your draw.
- Ignoring Symptoms: Don't get too fixated on the numbers alone. The entire point of considering what TRT is is to alleviate symptoms. A provider should treat the patient, not just the lab report.
When to Contact Your Doctor
You should always discuss your lab results with a doctor, regardless of what they show. Self-interpreting can lead to anxiety or incorrect conclusions.
Contact your doctor or a hormone specialist if:
- Your results for Total or Free Testosterone come back below the reference range on two separate morning tests.
- Your levels are "low-normal" but you continue to experience significant symptoms of low T.
- Your results show other abnormalities, such as high Estradiol or SHBG.
- You've received a diagnosis and want to understand your treatment options.
If low testosterone is confirmed, your provider will investigate the cause by looking at your LH and FSH levels. They can then discuss a plan which might include Testosterone Replacement Therapy (TRT). This is the stage where you'd learn about different delivery methods, like gels, creams, or injections. You would also discuss practical details like safe TRT injection locations and the differences between intramuscular and the increasingly popular TRT subcutaneous injection sites. Finding an online doctor that prescribes testosterone can be a convenient way to manage this process.
Ready to explore your options and speak with a licensed provider? The first step is getting matched.
Take our free 3-minute quiz to get matched with a top telehealth clinic for hormone therapy.
FAQs
How much does a testosterone test cost in 2026?
Without insurance, a basic Total Testosterone test costs around $69-$130. A more comprehensive panel including Total T, Free T, SHBG, and other markers typically ranges from $159 to $220 when ordered through a direct-to-consumer lab. With insurance, your out-of-pocket cost could be anywhere from a $0 copay to the full price, depending on your plan and deductible.
What is considered a low testosterone level?
The American Urological Association (AUA) uses a total testosterone level below 300 ng/dL as a reasonable cutoff to support a diagnosis, provided you also have symptoms. The Endocrine Society uses a slightly lower value of 264 ng/dL. However, many specialists focus on optimizing levels for symptom relief, not just hitting a minimum number.
Can I test my testosterone levels at home?
Yes, at-home test kits are available. They typically use a saliva sample or a finger-prick blood sample. While they offer convenience and privacy, their accuracy can be lower than a full venous blood draw performed at a certified lab. They are best used for a preliminary screening, not for a formal diagnosis.
What happens after I get my test results?
After getting two separate tests that confirm low testosterone, you should discuss the results and your symptoms with a doctor. If you are diagnosed with testosterone deficiency, your provider will discuss treatment options. These can range from lifestyle changes to hormone therapy, such as TRT injections or even alternatives like testosterone tablets for men.
If I start TRT, where are common injection sites?
If your doctor prescribes testosterone injections, they will teach you how to administer them safely. The most common TRT injection locations for intramuscular shots are the gluteal muscle (buttocks) and the ventrogluteal muscle (hip). Many patients now prefer TRT subcutaneous injection sites, which involve a smaller needle into the fatty tissue of the abdomen or thigh. Your provider will give you specific instructions.
Contributing to evidence-based peptide education and provider transparency.
Too many clinics, not enough clarity?
We don't sell peptides. Tell us your goals and we'll connect you with a vetted provider who can figure out what actually makes sense for you.
See what's right for youRelated articles
Which Protein Supplements for Muscle Growth Actually Work?
Tired of the hype? Find out which protein supplements for muscle growth are backed by science and learn how to pick the right one for your goals.
Hormone TherapyWhat Are the Real Magnesium Glycinate Benefits?
Uncover the science-backed magnesium glycinate benefits. We explore its effects on sleep, stress, and muscle function and explain why it's a top choice.
Hormone TherapyWhat B12 Shot Benefits Can You Actually Expect?
B12 shots are often hyped for energy, but the real b12 shot benefits are more specific. Learn who is a true candidate and what results to expect.